|
| Clara Bergen |
 |
| Lisa Bortolotti |
“We” are a group of six experts in philosophy, psychology, psychiatry, clinical communication, clinical practice, and public involvement in research (Interdisciplinary Academic Researchers), and five young people aged 17-25 with experience of accessing mental health services for diagnoses including post-traumatic stress disorder, major depressive disorder, generalized anxiety disorder, autism spectrum, and emotional dysregulation (Youth Lived Experience Researchers).
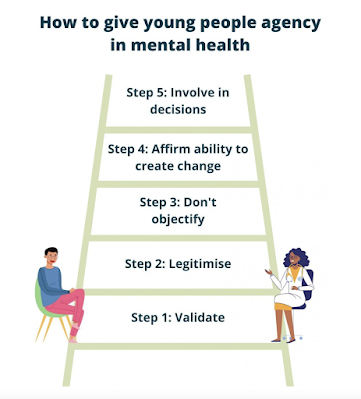
Both groups collaboratively analysed clips from video-recorded mental health encounters for young people seeking crisis support for self-harm or suicidal thoughts (see Bergen & McCabe 2021). During meetings in which the Youth Lived Experience Researchers watched and analysed video data, we identified what aspects of agency were most relevant to these mental health encounters. Five aspects of agency were thought to be important to young people but often undermined in the video-recorded mental health encounters.
1. is a subject of experience and their perspective matters;
2. can take action to change their situation by seeking help;
3. may have multiple and conflicting needs and interests;
4. with adequate support, can contribute to positive change;
5. with adequate support, can participate in decision-making.
1. An agent is a subject of experience and their perspective matters.
Validation is a critical tool for showing that the young person’s experiences and perspectives matter. A practitioner can show understanding and acceptance of the young person’s experience, without having to express agreement or approval. Some mental health assessments lack validation, as the main focus is on risk assessment and problem solving.
You need to say, “You’re really distressed. You’re in a lot of pain.” I think that kind of acknowledgement alone can be really, really powerful.
2. An agent can take action to change their situation by seeking help.
Legitimisation of help-seeking expresses that the young person made the right choice in seeking help. Communication techniques include for the practitioner to clearly state that the young person had genuine grounds for concern and deserves support. However, during assessments for suicidal thoughts, we observed that practitioners often implied that the young person didn’t need help, which could make them feel like they had no genuine concerns and did not deserve support.
With that sort of interaction, of “Oh you’re not planning to do anything now so it’s fine.” … You know, the department said it’s not an issue so it’s fine sort of having these thoughts… You wouldn’t think “Well maybe it’s really serious, maybe I do need to tell someone to help me.”